September 20 marks the first day of Advanced Practice Provider (APP) Week at Atrium Health. This third annual event combines five nationally recognized weeks of each individual APP profession into one fantastic celebration.
From Nurse Practitioners (NPs) and Physician Assistants (PAs) to Certified Registered Nurse Anesthetists (CRNAs), Clinical Nurse Specialists (CNSs) and Certified Nurse Midwives (CNMs) – APPs are an essential part of the patient care team. They create a seamless environment for patients and families, and are also integral to clinical research, mentoring and advocacy work.
The last year and a half have shown the immense strength, determination and grit our APPs exude on a daily basis. Their steadfast approach to patient care keeps our system going and we are endlessly grateful for the health, hope and healing they provide.
Below is a snapshot of our incredible teammates and the outstanding work they do each day. In honor of APP Week, please join us in expressing gratitude and celebrating all of our fantastic APPs this week (and always)!

Kathy Shaffer, CNS
Q1. What is your title and role at Atrium Health?
Clinical Nurse specialist supporting our Women's Service Line units at Carolinas Medical Center. I am also the CNS coordinator for the Central Division CNS team.
Q2. Why did you go into this field?
I’ve been a nurse for 23 years and have worked as a Clinical Nurse Specialist for the last four years. I completed my DNP in 2019 from Old Dominion University. As a nurse, I had the opportunity to work with some amazing CNS professionals and I was intrigued with their role and the impact they were able to have on patient outcomes. They inspired me to pursue the CNS pathway.
Q3. What do you find most rewarding about being an APP?
I love being able to use my training and critical thinking to dive into the evidence and really translate findings into practice. Being able to implement initiatives and processes that improve care, safety and the patient experience are the most rewarding parts of the job.
Q4. How has patient care impacted your life?
I have had the privilege to work with moms and babies for 22 years. My patients have taught me so much over the years and they continue to teach me. Being a part of both the happiest moments with new parents and also being by their side in the saddest moments have really taught me the value of life, the importance of compassionate care, and how powerful human touch and connection can be.
Q5. What has your experience been like as an APP during a pandemic?
The pandemic is unlike anything I have ever seen since becoming a nurse. The CNSs worked to develop crisis care standards that were shared across the system to help support all service lines in a crisis staffing situation. The CNS role is a unique APP role in that we work within all three spheres of impact – patient, nursing and organization/system. I’ve not only worked to improve patient care and patient-specific issues that came from COVID-19, but I’ve also had the change to create nursing care guidelines for COVID-19 patients (and system processes to support caring for these patients).
Q6. Do you have any projects or recent work that you showcased on behalf of Atrium Health?
I had a poster presentation at the North Carolina Affiliate of National Association of Clinical Nurse Specialists (NCNACNS) in August. The presentation highlighted a PI project on standardizing Pitocin administration to decrease postpartum hemorrhage. I also presented about Maternal Sepsis during the most recent Atrium Health Sepsis Series. As for my team, we published an article in the March – April 2021 Clinical Nurse Specialist Journal. Our article focused on the role of the CNS during COVID-19.
Q7. Can you share some personal moments of pride?
I am a mom of three kids – ages 20, 18 and 17! Another bright spot of mine is receiving a Tree of Life Coin for my work on our crisis care standards.
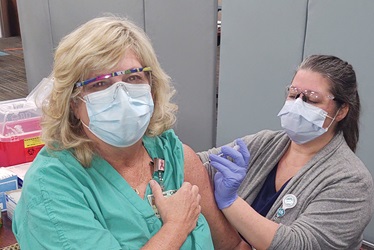
Kathy Shields, CNM
Q1. What is your title and role at Atrium Health?
I am a Certified Nurse Midwife at Atrium Health.
Q2. Why did you go into this field?
I graduated from the University of North Carolina at Chapel Hill in 1981 with a Nursing degree. That began my journey in Women’s health care. I worked as a labor and delivery nurse In Pinehurst, NC for 14 years prior to graduate school. I served as a charge nurse, Assistant Nurse Manager and Assistant Director of Women’s Health Care Services. As my role evolved through those years, I knew my career was to provide health care services directly to women. I entered graduate school at East Carolina University from 1993 to 1995 and obtained my MSN from the School of Nurse Midwifery. I completed some of my clinical rotations with CNMs in Pineville, which is how I was introduced to Charlotte. Charlotte OB/GYN was ready to start their first nurse midwife practice and I had the honor to develop that program with Dr. Jim Anderson, Dr. Bill McDonald, Dr. Craig Gourley, Dr. Maureen Beurskens, Dr. Larry Pixley, Dr. Alice Teague, and Dr. Robert Wicker.
Q3. What do you find most rewarding about being an APP?
I was the first Nurse-Midwife for Carolinas Medical Center (and at the time, Presbyterian Hospital Main). My days were busy providing care to obstetrical and gynecological patients, establishing office and hospital protocols, and embracing the medical community in this new role. For two years, I was the only CNM at the facility and provided on-call services 24/7. Today, we are an outstanding practice with seven CNMs. I knew the first years would be tough but the sacrifice was worth it. I was willing to embark on that journey to provide alternative services for women.
Q4. How has patient care impacted your life?
I’ve had the privilege to support the delivery of several teammates’ children. It is a truly full-circle experience and I love it! I’ve worked at Charlotte OB/GYN for the last 26 years and it is one of the most fulfilling aspects of my life. I have been on various committees, served on the North Carolina CNM Board and am a member of the American College of Nurse-Midwives. Giving back is important to me as well. I am a preceptor for many CNM and FNP students, along with serving as the Chief CNM for Charlotte OB/GYN. My work in not done yet – I hope we continue to grow the Nurse Midwife profession at Atrium Health.
Q5. Can you share some personal moments of pride?
I was introduced to my husband, Mike, by a labor nurse! We’re happily married for 18 years with two fur babies. I was not fortunate to have my own children, but I’ve had the privilege to assist mothers with the birth of over 2,000 kids. So, I have a community of children I cared for and am now seeing those young ladies as patients.

Mandy Castor, NP
Q1. What is your title and role at Atrium Health?
I am a family nurse practitioner, NP-C. I work as an APP at Northeast Women’s Health and Obstetrics. I also serve on the Women’s Service Line APP Committee.
Q2. What do you find most rewarding about being an APP?
My patients! I love being able to help women of all ages. I’ve held this position for 12 years and feel I’ve built great relationships with my patients. Their appreciation for the work I do is the reason I love my job. It is so rewarding, and those relationships help patients obtain the best care possible.
Q3. What has your experience been like as an APP during a pandemic?
The pandemic has changed a lot of our normal processes and procedures. Our teams had to adapt and continue moving forward. Last year, we were unable to allow family members into the office due to visitor restrictions. At that point, I felt like I became a stand-in family member (not just a provider) for patients. Now more than ever, I’ve worked to reassure my pregnant patients during the pandemic. Being a voice of peace and trust through these times is very rewarding.
Q4. Do you have a patient story that stays in your memory from this program? How did your care help that individual?
In the last class I taught, we had a new mom join who had only been home from the hospital for 48 hours. She was exhausted, struggling with breastfeeding and lack of sleep. She was having severe “mom guilt” and questioned if she was taking the best care of her newborn. Our class really encouraged her. The lactation consultant gave her pumping and breastfeeding tips. I was able to discuss sleep and baby blues with her. The other mothers shared their similar experiences and lifted this mother’s spirits. By the end of the session, this new mother was laughing and asking more questions. The group really fulfilled our goal to educate and support new mothers. It made my day to see the APP Committee’s dream of this class come to fruition and truly help a new mother.
Q5. Do you have any memorable projects or recent work that you showcased on behalf of Atrium Health?
I’m so proud of the 4th Trimester Support program created by the Women’s Service Line APP Committee. We developed these postpartum classes to help educate new moms and to also provide a way for mothers to meet each other. Classes are facilitated by an Advanced Practice Provider (CNM, NP or PA) who answers general questions in a group setting. New moms can share their birth stories, discuss breastfeeding concerns or offer tips, share how you are coping with your motherhood experience, and ask questions about birth control options.
It is an excellent opportunity to connect new mothers and help them build a community. Motherhood is challenging and exciting, but the adjustment can be overwhelming. The classes help mothers feel less alone through their experiences.
We’re also working on a pilot of the postpartum course with a cohort of moms over shorter periods of time. They meet over four sessions (instead of a single hour session) and focus on specific topics during each class.
Currently, classes are virtual due to the pandemic. We look forward to meeting in person when it is safe. For now, we encourage mothers to join virtual classes with their cameras on (and their babies on screen).

Chloe Greguska, PA
Q1. What is your title and role at Atrium Health?
I am an Inpatient Malignant Hematology/BMT PA.
Q2. Why did you go into this field?
I always knew I wanted to work in medicine because I wanted to make a tangible difference in people's lives. I was also interested in how the human body works. Being a PA is great for me because it’s a way to provide patient-focused care in an evidence-based way. I ended up in the oncology field solely through coincidence (from my fellowship) but am very thankful that is where I landed.
Q3. What do you find most rewarding about being an APP?
I can see the tangible impact of my decisions and care in the lives of the patients I treat.
Q4. How has patient care impacted your life?
I am inspired by my patients who remain positive, kind and grateful even on difficult days. It makes me more thankful for each interaction with my own friends and family.
Q5. What has your experience been like as an APP during a pandemic?
Overall, I felt the hospital system banded together to get through the challenges that come with a pandemic. I have a wonderful group of teammates that I can rely on for support.
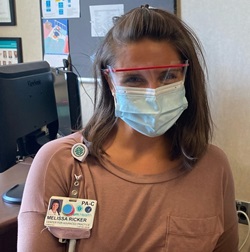
Melissa Ricker, PA
Q1. What is your title and role at Atrium Health?
My title is PA Fellowship Director (or Coordinator).
Q2. Why did you go into this field?
Following completion of my fellowship, I worked in Critical Care for a few years. During that time, I precepted students and discovered a passion for sharing the knowledge and skills I learned. That interest to get involved in the leadership of a larger fellowship brought me to Atrium Health. I started as the Medical Critical Care Coordinator before accepting my current role in 2018.
Q3. What do you find most rewarding about being an APP?
As a Critical Care PA, I really enjoy helping patients and their families at the intersection literal life and death. Driving a team that makes lifesaving decisions while providing family education is the most rewarding. Compassionate end-of-life care is also an essential component of critical care (when illness is no longer improving with medication, interventions and technology) and I am honored to facilitate these conversions with families.

Anne Vail, NP
Q1. What is your title and role at Atrium Health?
I am the NP Fellowship Director, overseeing operation of the APP Fellowship Program in tandem with Melissa Ricker. Also, I work clinically in Geriatric Medicine (in an ambulatory Memory Clinic) with the Senior Care team.
Q2. Why did you go into this field?
I love the concept of supporting APPs through a career transition, enhancing their clinical skillsets and building their leadership potential. Medicine is so rapidly changing. It is professionally fulfilling to prepare and support APPs for successful careers of lifelong learning.
Q3. What do you find most rewarding about being an APP?
Seeing the big picture and investing in someone's career ultimately funnels to great patient care. I love connecting with people and patients; understanding why and how they can be the best providers and train in the most optimal environments. We are all working to help people improve their health and wellbeing.
Q4. Do you have a patient story that stays in your memory? How did your care help that individual?
Learning a patient’s story is my favorite part. We all have our story to tell, and my patients tell me the best stories of their life. They share their accomplishments and observations of how the world has changed. It is important to listen. What makes a person tick? Did they serve in the military? Were they CEO of a company before retiring? Were they married for decades or recently lost a spouse? The human experience is vast and nuanced and endlessly interesting.
In patients with advanced dementia, I get the important opportunity to advocate and educate for the patient's quality of life. And just as each story is different, so too are their ideas of what this should look like. These discussions and decisions can be extremely difficult and personal.
Q5. How has patient care impacted your life?
There is an incredible responsibility as an APP. People, at their most vulnerable moments, are trusting you with their lives and futures.
Q6. What has your experience been like as an APP during a pandemic?
I think that the social isolation we have all experienced has required us to be more intentional about relationships and being creative to show people we care about them.
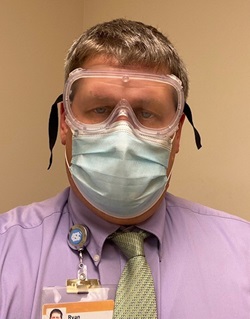
Ryan Vann, PA
Q1. What is your title and role at Atrium Health?
I am a Physician Assistant in Family Medicine at Atrium Health Wake Forest Baptist and a member of the Network Board of Managers.
Q2. Why did you go into this field?
I always knew that I wanted to take care of patients in some capacity. When I worked as a clinical laboratory scientist, I loved the science and technology aspect, but I wanted a role that allowed more direct interaction with patients. I also wanted the opportunity to personally work with patients and help them make good decisions about their health.
Q3. What do you find most rewarding about being an APP?
Where to begin? I love that APP education and APP practice naturally encourages team-based care. I appreciate the flexibility that is organically part of APP practice, such that moving from one specialty to the other is not only possible, but also openly encouraged. Another rewarding aspect of being an APP is the opportunity to provide leadership for and mentorship to other APPs both within and outside of Atrium Health.
Q4. Do you have a patient story that stays in your memory? How did your care help that individual?
Several come to mind, but one sticks out from early in my career. I saw a 10-year-old girl on a walk-in basis for vague abdominal pain. This was the first time I can recall having a true gut feeling that something was really wrong with a patient, and despite a somewhat atypical presentation, she was imaged and determined to have appendicitis. The team-based nature of our work was on full display that day – she was imaged quickly, she was seen in the ED immediately thereafter, and the surgical team took her to the OR within a few hours. By the time I went home that day, her appendix had been removed and she was doing well. I am fortunate that, years later, I still see her as a patient. She always introduces me to others as the “person who saved my life.” In reality, I played only a small part in that event, but I sincerely appreciate the special bond I have with this patient. The ability to create those relationships with patients and their families is so important to me as an APP in family medicine.
Q5. How has patient care impacted your life?
Many of my patients are also those whom I would consider friends. They ask about my family, we talk about our jobs, and we often share common interests outside of medicine. Often, I ask the patients I see in clinic about their relatives because they are also my patients. The ability to form multi-generational relationships with patients is one of the most rewarding aspects of what I do.
Q6. What has your experience been like as an APP during a pandemic?
My primary focus as an APP in a family medicine setting has been on keeping patients out of the hospital. We have done this not only by making sure COVID-19 patients are cared for, but also by ensuring that patients with chronic health conditions are appropriately managed. Those with chronic conditions then remain healthy and avoid the hospital.
I truly admire and appreciate the work that our colleagues in inpatient, emergency department, and urgent care settings have done as they have directly cared for patients who have consistently been very ill, often in significantly overwhelming numbers. I hope that our efforts to remove some of the strain from these colleagues has been helpful, and once again, I hope this emphasizes the importance of team-based care during this difficult time.
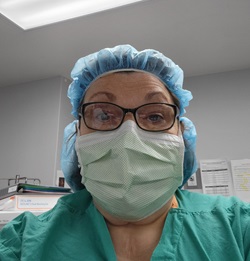
Sherry Bernardo, CRNA
Q1. What is your title and role at Atrium Health?
My title is Director of Metro Anesthesia Quality and Practice, where I support all Primary Enterprise facilities for practice and care improvement opportunities. I lead our quality and practice endeavors for the CRNA practice division and work with our MD colleagues for Best Practice opportunities on how we care for patients as they receive anesthesia (not only for operative cases but also for procedural and diagnostic testing). In addition, I continue to periodically provide anesthesia for patients in the OR and other sites throughout Atrium Health, caring for a very diverse patient population from neonates to the geriatric population.
Q2. Why did you go into this field?
I spent many years as an RN in various ICUs (STICU, CVICU, trauma and PACU). When I worked in Cardiac Surgery Recovery, I noticed the practice and presence of CRNAs. That exposure really clicked for me. I observed the collaboration and critical thinking skillet among unit RNs, surgeons and anesthesiologists.
Q3. What do you find most rewarding about being an APP?
The ability to work as part of an interdisciplinary team is most rewarding to me. I have the opportunity to utilize my advanced critical thinking skills and care for patients when they are most vulnerable…under anesthesia and not able to make decisions for themselves.
Q4. Do you have a patient story that stays in your memory? How did your care help that individual?
I have many stories where I have cared for individuals who are experiencing lifechanging events. It’s always a great feeling when patients put their trust in me (especially when I only have five or ten minutes to meet them prior to their OR trip). Bringing a child to the OR and leaving their parent can often be the most trying time in our practice. I cannot imagine the stress and anxiety the parent is experiencing as we walk away with their child. I need to instill trust, as well as skill and compassion with a limited time to do so.
Q5. How has patient care impacted your life?
I grew up with a mother that was in nursing for the majority of her adult life. So, caring for others was instilled in me very early on and I knew that was a career path I wanted to pursue. Prior to nursing, I considered a career in veterinary medicine and actually have an undergraduate degree in Animal Bioscience. However, I quickly realized that the tug on my heartstrings would make this a difficult career and turned my attention to the nursing field. Not a day goes by that I regret my decision with my career path.
Q6. What has your experience been like as an APP during a pandemic?
The pandemic has certainly opened my eyes to the many areas that can be impacted by my role as an APP. From planning how to safely deliver anesthesia to patients and leading our department in COVID-19 safety initiatives with my MD chiefs, to supporting surge efforts with CRNA care to supplement other disciplines. As a CRNA, I have the unique ability to channel my skillset into many practice settings – even outside the OR.



